Chronic obstructive pulmonary disease (COPD) affects many people globally, causing distress to patients and families and burdening healthcare systems. It is a challenging disease to manage. According to studies, COPD hospitalizes approximately 700,000 individuals in the United States annually. Data also shows that these individuals have a readmission rate of over 20% within 30 days.
Advancements in technology now allow for remote monitoring of COPD patients. This has resulted in improved disease control, earlier treatment, and better outcomes. Remote patient monitoring solutions also offer an effective way to reduce healthcare costs.
How can healthcare providers remotely monitor COPD patients?
Below are among the most common ways that clinicians are monitoring and managing their COPD patients:
Pulse Oximetry. Pulse oximeters, non-invasive devices, have improved COPD care. They enable care teams to track patient blood oxygen saturation levels regularly and get feedback in real-time. This proactive approach allows for detection of respiratory distress and prompts timely intervention. However, it’s important to note that a drop in blood oxygen levels often occurs when COPD exacerbations are already moderate or severe (source).
Pulmonary function tests (PFTs). Measuring lung volume and spirometry have played a crucial role in monitoring lung function in COPD patients and it is now possible to do this remotely. Consistent use of PFTs help doctors detect worsening lung function and adjust treatment plans accordingly. One challenge with PFTs is that it is subject to patient error and are mainly used to monitor the progression of COPD rather than exacerbations.
Smart inhalers and medication management. Smart inhalers, equipped with sensors, offer real-time data on medication usage, adherence, and inhaler technique. These connected devices sync with smartphones or tablets, empowering COPD patients to take control of their treatment. While this approach can prevent hospitalizations, it does not allow for directly assessing patient vitals or symptoms.
Patient Self-Reporting of Symptoms. Symptoms like coughing, wheezing, and shortness of breath are considered the early warning signs of exacerbations. Patients can report their symptoms using electronic diaries (eDiaries), facilitating earlier interventions. However, it is difficult for patients to keep track of their symptoms, leading to inconsistent reporting and false alerts.
Virtual consultations: Telehealth has transformed healthcare delivery by offering virtual consultations for COPD patients, allowing for more consistent communication. Virtual consultations can allow for regular assessments that can lead to treatment adjustments and guidance to patients. While virtual consultations can be effective, they are time-consuming for care teams.
The RESP Biosensor: An Innovative Technology for COPD Remote Patient Monitoring
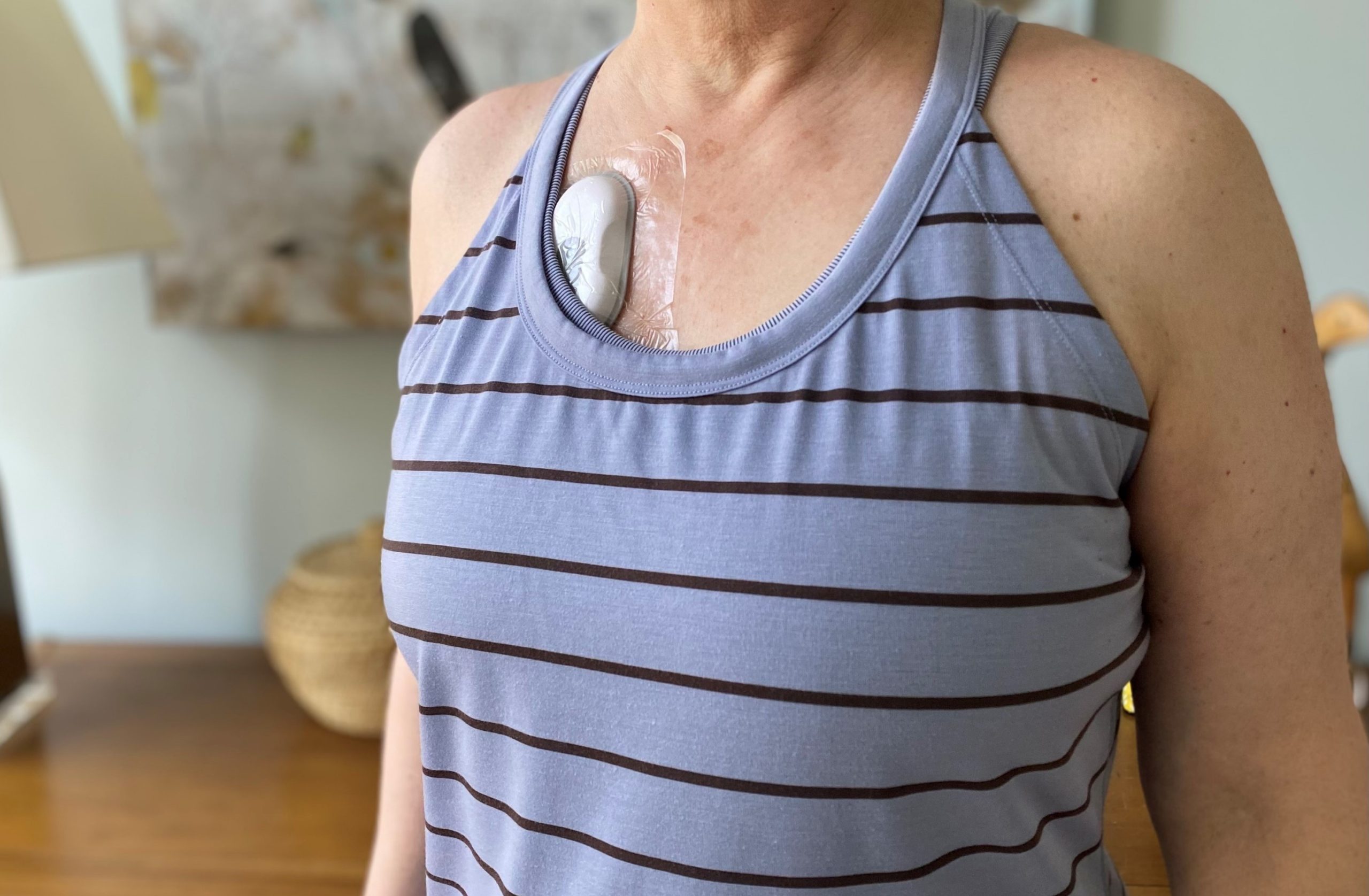
The RESP Biosensor, an FDA-cleared wearable device developed by Strados Labs, offers a new approach to COPD management. By continuously capturing lung sounds, similar to a stethoscope, it allows clinicians to objectively monitor changes in coughing and wheezing—early warning signs of COPD-flareups.
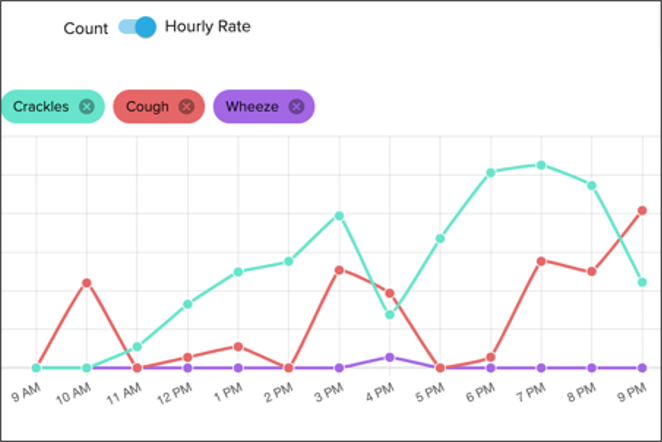
Doctors can prescribe the device to the pulmonary patients that they want to manage remotely and patients wear the device while at home. Lung sound data captured by the device are transferred to a clinician portal where care teams can see changes in cough and wheeze rates.
Our research has shown a relationship between abnormal lung events and hospitalizations. The technology has the potential to give clinicians earlier insight into exacerbations, provide an objective way for clinicians to measure the care plan against, and relieve patients of the burden of tracking these symptoms constantly.
Conclusion
The emergence of COPD remote monitoring devices has helped improve disease management, reducing unnecessary hospitalizations and improving patient quality of life. By embracing these technologies, clinicians can better monitor respiratory health and help break the cycle of readmissions.
As the RESP Biosensor and other devices continue to gain wider acceptance, the promise of remote monitoring in transforming the lives of COPD individuals becomes increasingly evident.